“Stage 2…”
“Stage 4…”
Those words feel like the ground has just dropped from under you.
And for many, it quickly becomes the focus. Families start searching online, comparing stories, and jumping to conclusions.
Doctors use staging as a kind of map, not a verdict, telling them where the cancer is, how far it has spread, and what kind of treatment might work best.
Two people can both have “Stage 3 cancer,” and yet have very different situations. That’s because staging is just one piece of a much bigger picture.
In this post, we’re going to look at the different nuances of cancer stages.
Because once we understand what they mean (and don’t mean), the situation can begin to make a lot more sense.
What Is Cancer Staging?
Cancer is a group of diseases where abnormal cells grow uncontrollably and may invade nearby tissues or spread to other parts of the body. Some cancers form tumors, while others do not.
And staging is simply a way of answering questions like: “How much cancer is there, and where is it?”
Think of it like tracking a typhoon. When a storm enters the Philippines, we don’t just say “There’s a typhoon.” We ask: Where is it now? How strong is it? Which areas are affected? Where is it heading? That’s what staging does…but for cancer.
Cancer staging describes:
The size of the tumor
Whether it has spread to nearby lymph nodes
Whether it has reached other parts of the body
This matters because cancer doesn’t stay still. Some grow slowly and remain in one place for years, while others move early and spread through the different parts of the body.
What Doctors Do To Determine The Stage?
The number doesn’t just come out of thin air. It’s built step by step (sometimes over days, sometimes weeks) using different tests and procedures that each reveal a part of the picture.
No single piece of evidence is enough on its own. But put together, they build the case.
Here are some of the things doctors do to investigate the situation.
#1 Lab Tests and Biomarkers
Blood tests don’t usually determine stage on their own, but they provide plenty of information.
Some cancers release specific markers into the blood, so we look for these markers through lab testing. Other cancers can affect organ function, and this can show up in lab results.
Advanced testing can also identify specific targets for therapy, which is an important feature of modern cancer care.
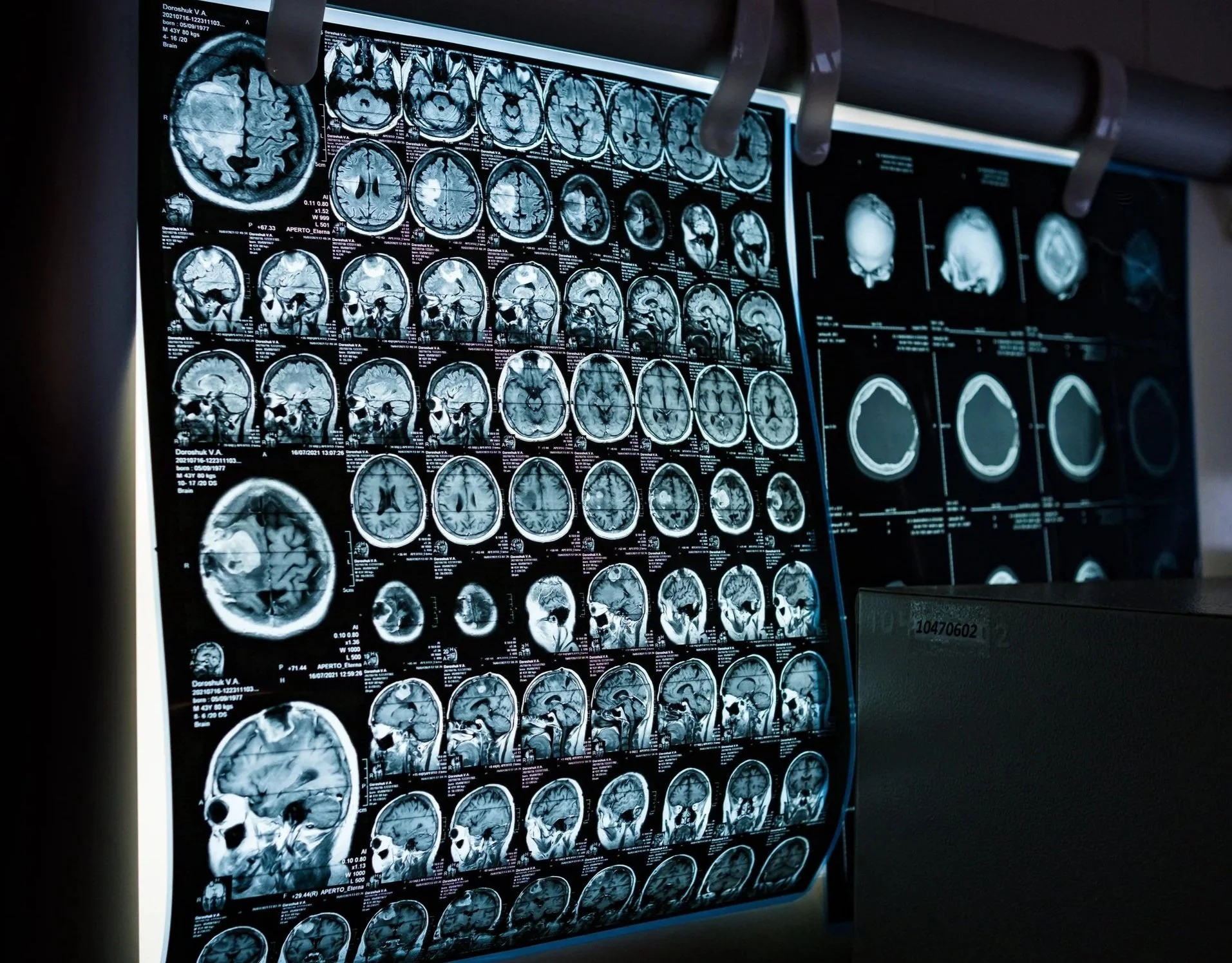
#2 Imaging: Seeing Inside the Body
Depending on the situation, the doctor may ask for any of the following:
CT scans
MRI
PET scans
These help doctors see where the tumor is, how big it is, and whether there are signs of spread.
For example, a CT scan might show a mass in the lung. A PET scan can then highlight areas where cancer cells are more active, showing “hotspots” that light up.
#3 Biopsy: Confirming What It Is
Imaging can suggest cancer, but it can’t confirm it.
That’s where a biopsy comes in. This is when a small sample of tissue is taken and examined under a microscope.
Through biopsy, doctors determine if a tissue sample is benign (non-cancerous) or malignant (cancerous). A pathologist examines the cells under a microscope to identify abnormalities and provide crucial information.
In some cases, surgery is done. The tumor itself is removed and examined closely, leading to a more precise pathological staging.
So, what have we learned so far?
We learned that no single test gives you a stage. Doctors combine lab tests, imaging results, and biopsy findings.
Because of this, staging can sometimes take time. Not because doctors are unsure, but because there are many things to do to get the whole picture.
So how do doctors actually determine the stage?
Doctors use the TNM system.
TNM stands for:
T (Tumor) – How big is the main tumor? Has it grown into nearby tissues?
N (Nodes) – Has the cancer spread to nearby lymph nodes?
M (Metastasis) – Has it spread to distant organs like the lungs, liver, or bones?
Each letter gets a number attached to it. For example, a tumor might be labeled “T2 N1 M0,” which sounds intimidating, but it just means:
Medium-sized tumor
Some lymph node involvement
No distant spread
Doctors then combine these details to assign an overall stage (1 to 4).
This system is used worldwide and is maintained by organizations like the Union for International Cancer Control (UICC) and the American Joint Committee on Cancer (AJCC).
The 4 Cancer Stages Explained
Okay, so let’s now talk about the part most people latch onto.
The number: Stage 1, 2, 3, or 4.
What does each stage mean?
Stage 0: The Earliest Form
Stage 0 is often left out of conversations, but it matters.
This is called “carcinoma in situ,” a stage when cancer cells are present, but they haven’t invaded any nearby tissues yet. In short, they’re still contained.
Because of that, treatment is often highly effective. And in many cases, removing the abnormal cells early can prevent them from becoming worse.
This is why regular screening programs are so important. The World Health Organization emphasizes that early detection of pre-cancerous lesions significantly reduces cancer incidence and mortality. For example, early-stage cervical changes detected through screening can often be treated before they develop into full-blown cancer.
Stage 1: Localized and Contained
Stage 1 means the cancer is small and still confined to where it started. It hasn’t spread to lymph nodes or distant organs.
Because of that, treatment is often straightforward:
Surgery is usually the main option
Sometimes followed by radiation or medication, depending on the type
Outcomes at this stage are generally favorable. For many cancers, early-stage detection is linked to significantly higher survival rates. For instance, localized breast cancer has a 5-year relative survival rate of about 99%, according to data from the American Cancer Society.
Again, this reflects the importance of coming in for regular screenings to catch things at the earliest stages.
Stage 2: Growing, But Still Local
Stage 2 usually means one of two things:
The tumor is larger, or
It has started to involve nearby lymph nodes
It’s still considered relatively localized, but the cancer is showing signs that it’s more active.
Lymph nodes are small, bean-shaped structures of the lymphatic system, which help your body fight infections and maintain fluid balance. We have lymph nodes all over the body, like in the neck, armpits, chest, abdomen, and groin.
Cancer cells can break away from a tumor and travel through the lymph fluid. They often get trapped in nearby lymph nodes. They’re one of the first places cancer spreads.
Doctors check on the lymph nodes because if cancer shows up there, it suggests it’s starting to move beyond its original site.
In Stage 2, treatment often becomes more layered:
Surgery
Plus chemotherapy or radiation to reduce the risk of recurrence
The key idea here is containment with caution. Doctors are already thinking ahead, “Let’s stop it from spreading.”
Stage 3: Regional Spread
Stage 3 cancer has spread beyond the original site to nearby lymph nodes or surrounding tissues, but not to distant organs.
This is what doctors call locally advanced cancer.
At this point, treatment is usually more aggressive and combined:
Surgery (if possible)
Chemotherapy
Radiation
Sometimes targeted or immunotherapy
It’s not just about removing the tumor anymore. It’s controlling a wider area.
A large analysis in The Lancet Oncology showed that survival rates drop as cancer spreads regionally, but outcomes still vary widely depending on cancer type and treatment response.
So Stage 3 is serious…but far from hopeless.
The survival rates at this stage vary.
Stage 4: Metastatic Cancer
Stage 4 means the cancer has spread to distant parts of the body, like the lungs, liver, bones, or brain.
This is what people often fear the most, and it’s also the stage that’s most misunderstood.
The goal of treatment often shifts from cure to:
Control
Prolonging life
Maintaining quality of life
But here’s the part many don’t hear enough:
Stage 4 does not automatically mean “end of the road.”
With newer treatments (eg, especially targeted therapy and immunotherapy), patients are living longer than before. Advanced cancers can be managed for years, almost like chronic conditions.
For example, studies have shown significant survival improvements in metastatic melanoma and lung cancer, with no apparent loss of quality of life in the patients.
But knowing the cancer stage, even if it comes from a battery of tests and procedures, still doesn’t give us the whole picture. Here’s why…
Why Staging Is Not the Whole Story
It’s tempting to treat a cancer stage like a final answer.
But not really.
Here are three reasons why:
#1 Same Stage, Different Realities
Let’s say two patients are both diagnosed with Stage 4 cancer. On paper, that sounds like the same situation. In reality, it can look completely different.
Take breast cancer versus pancreatic cancer. Both can be Stage 4, but survival outcomes vary widely.
According to global cancer data compiled in CA: A Cancer Journal for Clinicians, metastatic breast cancer patients can live several years with treatment, while pancreatic cancer tends to be more aggressive, with shorter survival times
Same stage. Very different diseases.
Even within the same cancer type, differences still show up.
#2 Biology Changes Everything
“What kind of cancer is this, exactly?”
Tumors have their own biology…like their own personality. Some grow slowly. Some respond well to specific drugs. Others don’t.
For example:
Certain breast cancers with HER2-positive markers respond well to targeted therapy
Some lung cancers with EGFR mutations can be treated with oral medications instead of traditional chemotherapy
By molecular profiling, cancer treatment has vastly improved through therapies tailored to genetic mutations rather than just stage
So two patients with the same stage might receive completely different treatments (and have different outcomes) because their cancers behave differently at the cellular level.
#3 Personal Matters: Individual Differences
Age, overall health, access to care, and even support systems can influence outcomes.
In the Philippine setting, someone diagnosed in a major medical institution may have access to advanced diagnostics and newer treatments, while those in less-than-ideal settings might face delays or limited treatment options.
Timely diagnosis and treatment significantly affect survival rates, sometimes as much as the biology of the disease itself.
The stage tells you where the cancer is. But it can’t guarantee answers to questions like:
How fast will it grow
How well does it respond to the chosen treatment
So staging is not the full story.
Biology, context, and technology play a part, too. And patients never had this much optionality and high-level care.
Receiving a stage diagnosis guides the next steps.
Treatments Have Come A Long Way
What used to be true about cancer even 10 years ago doesn’t always hold true today.
Immunotherapy, targeted drugs, and combination treatments have brought positive outcomes for many advanced cancers. Patients who might have had very limited options before now have more pathways.
While staging gives structure, direction, and a starting point, it’s not destiny.
Treatment decisions are shaped through tests, ongoing conversations, adjustments, and trust. Cancer is best approached through partnership with your doctors.
BloodWorks Lab provides you with quick and accurate laboratory tests that help you and your care team make timely and well-informed decisions. We are your healthcare partners.
Book your appointment today.
Our branches are in Alabang, Katipunan, and Cebu.